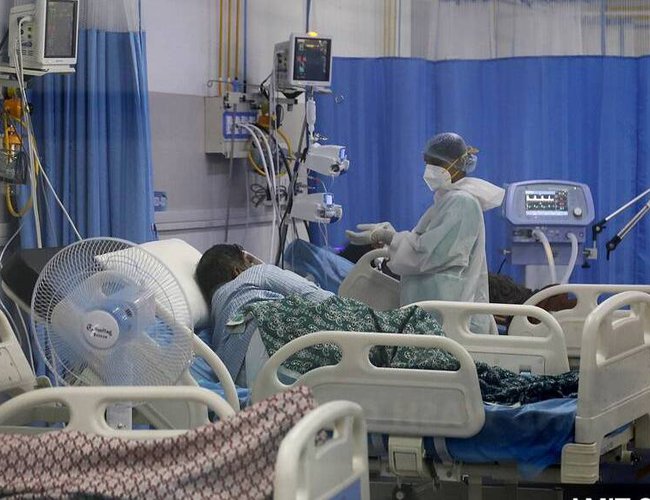
The Context
From mid-April 2021, Nepal has been facing a second wave of coronavirus infections. The numbers of new infections and deathshave spiked and the pandemic has created what some see as a ‘pathetic situation’.Hospitals faces shortages of adequatelytrained technicians, health equipment, beds, medicines, medical oxygen, and so forth. Towns close to the Indian border have been the hardest hit by the health emergency as the number of cases continues to skyrocket.
To manage this adverse situation, on April 19, the Nepaligovernment imposed a number of restrictions on public movements and gatherings in many cities, including those close to the border with India, and canceled all domestic and international flights. It also instructed provincial and local governments to take necessary measures to check the spread of the coronavirus, including the creationof isolation facilities andquarantine and holding centers along the Indian border.
On May 11, a total of 9,483 new infections and 225 deaths were reported, a record single-day spike. HEOCrecords revealed that,as of May 16,at total of reverse transcription polymerase chain reaction (RT-PCR) is 2,770,980, RT-PCR test million is 95,102, total positive case (PCR) is 455,020 and total confirmed cases in isolation are 110,263. Total recovered cases are 339,756 and recovery rate is 74.7%. A total of5,001people had died. Also as of May 16, 701 people were in quarantine, 102,455 people were in home isolation and 7,808 were in institutional isolation. The number of patients in ICUs and on ventilators were 1,313 and 380 respectively.
Nepal’s COVID-19 response is being carried out under the leadership of25 hub hospitals across Nepal, but many of them are still ill-prepared. The lack of coordination among the local, provincial and federal governmentsand political turmoil have weakenedthe healthcare system as a whole. With limited capacities, hospitals have stopped admitting new patients. In fact, Nepal’s healthcare system is quite fragile. HEOC records reveal that it has only 1,595 intensive care beds and480 ventilators and only 0.7 doctors per 100,000for its total population (about 30 million).
Along with Kathmandu Valley, the severity of COVID-19 in Lumbini, Sudurpaschim and Karnali provinces in general, and the cities of Nepalgunj, Dhangadhi and Butwal in particular, is great due to the considerable number of positive tests and the high inflow of people returning from India. Many humanitarian agencies (the UN, Nepal Red Cross Societyand civil society organizations) and the private sector haveextended their hands to support provincial and local governments in preventing infection and managing cases by providing surgical masks, disposable gloves, hand sanitizer, blankets, mosquito bed nets, packets of oral rehydration salts, as well as tents to establish quarantine and fever clinics.
At a time when many other hub hospitals were in a dilemma over how to respond to the surge in coronavirus patients with limited resources, the Bheri and Seti hub hospitals in NepalgungandDhangadhi respectively areresponding to COVID-19 systematically.Below are some of the crucial supporting factors behind this success as well as the challenges that lie ahead.
Supporting factors
Several mechanisms helpedBheri and Seti hub-hospitalsto facilitate the COVID-19 response in Banke and Kailali districts along with their large catchment areas. Good coordination, awareness campaigns regarding emergency care management;a series of capacity-building initiatives, including emergency trauma and ambulance management; responsive local government and provincial health offices; a good referral mechanism; qualified hospital preparedness for emergencies(HOPE)graduates; and well-capacitated provincial HEOCs were some of the key initiatives for improving response readiness. In addition, good coordination between health teams and municipal authorities and high levels of morale, dedication and ethical behavior among healthcare staff were key to success.
A series of awareness exercises on preparedness and preparation for a potential pandemic through full-scale simulation exercises, review-and-reflection sessions, media advocacy, and other approacheshelped to build clarity among the stakeholders about what to do and what not to do during the emergency period.With the support of a series of capacity-building initiatives (through training, drills, and simulation exercises), hospital management and staff have not only been sensitized to preparedness for mass events but also acquired a thorough knowledge and myriad skills related to preparedness, the referral mechanism, first aid, primary trauma care, and emergency trauma management. Increased awareness about the rationale behind the referral mechanism amongst female community health volunteers (FCHVs) helped a lot. Community resilience has been enlarged by strengthening the capacities of community members, including FCHVs and nurses, in first aid and emergency referral for health sector emergency preparedness and disaster response readiness. Training in primary trauma care and emergency trauma management helped to build health workers’ confidence about managing mass casualty incidents. The skills and knowledge gained from the training were widely used during the response to COVID-19. Building the capacities of emergency health volunteers through training, drills, and simulation exercises, strengthening the mechanism of coordinating between hub and satellite hospitals networks and health partners, and the creation of appropriate linkages with pre-hospital and post-hospital emergency care has resulted in the timely management ofCOVID cases.
The provision of training in first aid as well as the safe transport of patientsto ambulance drivers and some community emergency medical technicianswas instrumental in fostering the safety of all involved. Meetings of ambulance networks, monitoring of ambulance services, and pre-hospital conferencing collectively helped to strengthenambulance services and networks though there is still much leftto systematize.
Local governments and provincial health offices are gradually taking on the role of managing outbreaks and other incidentsdespite the limited number of public health staff and scarcity of financial resources. Introducing a referral mechanism (both protocol and pathway) in Banke and Kailali districts was done to more closely link pre-and post-hospital care with hospital care. Despite much effort, however, the frequent transfer of staff and inadequate allocation of resources has hindered the scaling up of preparedness initiatives. That said, the involvement of government and other relevant stakeholders can endorse and improve the referral management.
Bheri and Seti hospitals have begun to exercise their skills in handling mass casualty events, including the management of COVID-19. These hubhospitals crafted hospital disaster preparedness and response plans and operationalized their plansto address the ongoing response. The periodic meetings and review-and-reflection sessions held by the hubhospitalsand their satellite networks further helped to operationalize the plans by leveraging human and financial resources.PHEOCs in Karnali and Sudurpachhim provinces were established with the technical and financial assistance of the WHO,which has contributed a lot to the COVID-19 response. The roles of these PHEOCs in health information management and coordination, as well as disease surveillance and COVID logistics management, were praiseworthy. They successfully coordinated and managed the dengue outbreak response in 2019. Provincial Health Directorates have allocated some funds for the institutionalization of PHEOCs. Theinformation management officers at Banke and Kailali DEOCs agree that the good coordination and information management for COVID-19 response was as a result of the PHEOCs’ working hand-in-hand with DEOCs and LEOCs.
The majority of these supporting factors were generated as an outcome of the DIPECHO IX project, entitled “Strengthening the Emergency Response Capacity of Critical Hub Hospital Networks in the Mid- and Far-Western Development Regions of Nepal,” which ran from May 2017 to February 2019 and was based on the experiences and outcomes of three earlier DIPECHO project cycles in Kathmandu Valley between 2011 and2016. The project was implemented by the WHO in association with Merlin/Save the Children, Oxfam, Danish Red Cross and Handicap International with funding support from European Commission Humanitarian Aid (ECHO).
While the COVID-19 response has been well-managed, some challenges still linger and threaten to undermine its success.
Challenges
Some factors challenged the systematization of the COVID-19 response. Limited human and financial resources, limited equipment, high staff turnover, the absence of a threshold for the mobilization of response teams from the provincial and federal levels, the absence of understanding of the hub and satellite hospital network system, inadequate knowledgeabout HEOC and its functions at the department and division levels, and costs related issues to emergency referrals to hospitals were some crucial challenges.
While a series of training events have strengthened the capacities of primary responders, limited ambulance networks, resources and equipment as well as the high turnover of trained human resourcesmeant that hub and satellite hospitals were not able to provide hospital care services as expected.The transition of the healthcare structure as a result of federalization contributed to there beinginadequate staff, frequent staff changes and movements from federal to province to district and local hospitals, delays in real-time reporting, and slow implementation of newly endorsed guidelines and protocols. Shortages of hospital technical and administrative staffhave also hinderedCOVID-19 response.Not all hub hospitals have the largest capacity in their catchment areas. The key role of a hub hospital is facilitation and coordination with the federal ministry for appropriate response support. In Banke, for example, the capacity of Nepalgunj Medical College, a satellite hospital, is larger than that of Bheri hospital, a hub. In general, the flow of patients largely depends upon the proximity of a hospital to the point of incidence; whether the hospital is a hub or a satellite hospital is immaterial. The harmonious relationships between hub and satellite hospitalsand uniform understanding about the roles and responsibilities of HEOCshelp create an appropriate atmosphere for uplifting health sector emergency preparedness and response initiatives. Limited resources for the referral mechanism and for a systematic plan to build the capacityof district disaster response teams (DDRT), staff turnover and limited commitment from hospital management personnel also undermine effective response.
There are costs related to emergency referrals to hospitals, especially for ambulance services (land and air). People who can afford it may go directly to the hospital, while families with fewer resources tend to use primary health care facilities or the services atthe nearest health facility. The capacity for primary healthcare facilities to provide emergency care services islimited. The difficulty poor people face in accessing care is contrary to the concept that emergency care is an essential element of universal health coverage. There is a need to uphold equity by providing non-discriminatory access to all people in need of timely care, whether or not they are able to pay the cost. Because there are inadequate trained staff, poor prevention and control of hospital infections, limited ICU bed capacity and inadequate equipment and supplies the effectiveness of the COVID-19 response has been undermined.
A referral mechanism (both protocols and pathways) was introduced in Banke and Kailaidistricts to more closely link pre-and post-hospital care with hospital care but these referral protocols and pathways are new for all stakeholders, including NRCS. The replacement of the existing referral protocol with the new protocol through behavior change communication was a challenge. Though DDRTs were provided with standard operating procedures, the number of trained DDRT is limited, rosters are not periodically updated and disseminated, and no refresher training is provided. Unless the rosters of volunteers are periodically updated and disseminated through PHEOCs, DEOCs and other stakeholders, volunteers will not be mobilized instantly during emergency responses. The frequent turnover of staff, especially in hub hospitals, created a state of confusion and lead to the loss of the 'institutional memory' of the hospitals. This loss as well as limited commitment from hospital management also decreased the effectiveness of the COVID-19 response.
Immediate next steps
Online discussions with stakeholders revealed that the recommendations of the DIPECHO IX Project are still validand can contribute to a systematic response to COVID-19. In order to systematize the COVID-19 response and make it more holistic, there is a need to review the commodities to be stockpiled at hospitals with more focus on commodities with long shelf-lives, including surgical consumables & PPE and less focus on pharmaceuticals. There is also need to be more adequate buffer stocks of essential medicines and commodities in every hospital targeting diseases outbreaks such as COVID-19.For this, a dedicated staff member needs to manage the emergency logistics warehouse at the hospital.
The establishment of a mechanism for the everyday emergency care system in the hospitals is a crucial need as emergency care is an important component of universal health coverage. Everyday emergency care systemscould be managed throughbetter organization of theflow of patients, the training and mentoring of staff, and a hospital infection prevention and control mechanism.Simulation exercises involving all health sector stakeholders (pre- and post-hospital care), ambulances, security agencies and municipal and district officials, are very usefulin putting to the test existing preparedness and response readiness and thereby in improving the chain of emergency care from the community to the hospital.
The role of Provincial HEOCs is paramount in responding to the COVID-19 outbreak. ProvincialHEOCs must have the capacity to undertake testing and contact tracing and, in collaboration with provincial health authorities,take necessary communal interventions. There is a need to build the technical capacities of ProvincialHEOCs, paying special attention to disease outbreaks and investigations; risk assessment and risk communication; allocation of sufficient financial resources; epidemiology, preferably through field epidemiology training; and a robust coordination and mechanism for information-sharing among provincial health authorities, hospitals and other health facilities. Support for ProvincialHEOCsfor providing training on the protocols for early investigations, the control of hospital infections, and case management is equally important. There is a need to conduct COVID-19 table-top exercises using theWHO package and to facilitateon-line training for hospital management and clinical staff.Along with building the institutional capacities of ProvincialHEOCs, the development of a policy for better integration of pre-hospital care, including ambulance services, into the healthcare systemis key. Before such a policy is in place, however, the number of ambulances with paramedics (Cat A&B) needs to be increased and the links between ambulance services and hospitals need to be closer.
(Dr. Gautam is an Independent Researcher and Consultant. He is associated with National Disaster Risk Reduction Centre (NDRC) Nepal as Senior Research Fellow and HARDI/Western Sydney University as Adjunct Fellow. He can be reached through drrgautam@gmail.com.Mr. Adhikari is associated with WHO as National Professional Officer for Emergency Preparedness and Response. He can be reached through adhikarid@who.int)
















