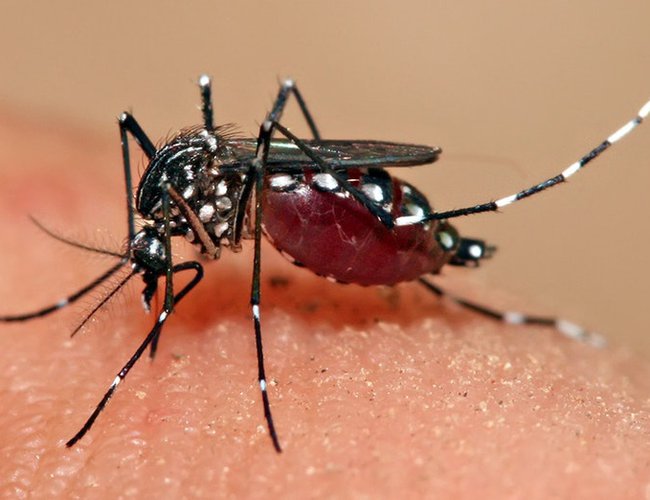
Dengue fever is a mosquito-borne tropical disease caused by the dengue virus. The virus has five types; infection with one type usually gives lifelong immunity to that type, but only short-term immunity to the others. Subsequent infection with a different type increases the risk of severe complications. Symptoms typically begin three to fourteen days after infection. This may include a high fever, headache, vomiting, muscle and joint pains, and a characteristic skin rash. Recovery generally takes two to seven days. In a small proportion of cases, the disease develops into severe dengue, also known as dengue hemorrhagic fever, resulting in bleeding, low levels of blood platelets and blood plasma leakage, or into dengue shock syndrome, where dangerously low blood pressure occurs.
Dengue has become a global problem since the Second World War and is common in more than 110 countries, mainly in Asia and South America. Each year between 50 and 528 million people are infected and approximately 10,000 to 20,000 die. The earliest descriptions of an outbreak date from 1779. Its viral cause and spread were understood by the early 20th century.
Most people with dengue recover without any ongoing problems. The fatality rate is 1–5%, and less than 1% with adequate treatment; however those who develop significantly low blood pressure may have a fatality rate of up to 26%. In 2013 it caused about 60 million symptomatic infections worldwide, with 18% admitted to hospital and about 13,600 deaths. For the decade of the 2000s, 12 countries in Southeast Asia were estimated to have about 3 million infections and 6,000 deaths annually. It is reported in at least 22 countries in Africa; but is likely present in all of them with 20% of the population at risk. This makes it one of the most common vector-borne diseases worldwide.
Infections are most commonly acquired in the urban environment. In recent decades, the expansion of villages, towns and cities in the areas in which it is common, and the increased mobility of people has increased the number of epidemics and circulating viruses. Dengue fever, which was once confined to Southeast Asia, has now spread to Southern China, countries in the Pacific Ocean and America, and might pose a threat to Europe.
Rates of dengue increased 30 fold between 1960 and 2010.This increase is believed to be due to a combination of urbanization, population growth, increased international travel, and global warming. The geographical distribution is around the equator. Of the 2.5 billion people living in areas where it is common 70% are from Asia and the Pacific.
Dengue fever cases have been reported every year from southern lowland Tarai in Nepal since its emergence in 2004. In 2010 and 2013, Nepal experienced two large outbreaks with 917 confirmed cases and five deaths, and 642 confirmed cases respectively. Lowland Tarai especially Chitwan and Jhapa district were severely affected districts in those outbreaks. Recently the disease has been reported from higher elevated mid hills. This year in May second city of Dharan experienced the unexpected outbreak. Nepal is one of the vulnerable countries from the global climate change perspectives. The region has warmed up by 1.5 °C in the last 25 years with much higher rates compared to the global average and is expected to be warmer and wetter in the future due to climate change. In this context dengue is likely to be shifted toward higher elevation in response to such climate change. The recent study documented the presence of A. aegypti up to 2000 m above sea level and all the serotypes of dengue virus circulate among host, vector and environment in the country. The dengue problem can be anticipated to get much worse in the future. An infection with dengue is second only to malaria as a diagnosed cause of fever among travelers returning from the developing world. It is the most common viral disease transmitted by arthropods, and has a disease burden estimated at 1,600 disability-adjusted life years per million population. The World Health Organization counts dengue as one of seventeen neglected tropical diseases.
Typically, people infected with dengue virus are asymptomatic (80%) or have only mild symptoms such as an uncomplicated fever. Others have more severe illness (5%), and in a small proportion it is life-threatening. The incubation period (time between exposure and onset of symptoms) ranges from 3 to 14 days, but most often it is 4 to 7 days. Therefore, travelers returning from endemic areas are unlikely to have dengue if fever or other symptoms start more than 14 days after arriving home. Children often experience symptoms similar to those of the common cold and gastroenteritis (vomiting and diarrhea) and have a greater risk of severe complications, though initial symptoms are generally mild but include high fever.
The characteristic symptoms of dengue are sudden-onset fever, headache (typically located behind the eyes), muscle and joint pains, and a rash. The alternative name for dengue, "breakbone fever", comes from the associated muscle and joint pains. The course of infection is divided into three phases: febrile, critical, and recovery.
The febrile phase involves high fever, potentially over 40 °C (104 °F), and is associated with generalized pain and a headache; this usually lasts two to seven days. Nausea and vomiting may also occur. A rash occurs in 50–80% of those with symptoms in the first or second day of symptoms as flushed skin, or later in the course of illness (days 4–7), as a measles-like rash. A rash described as "islands of white in a sea of red" has also been observed. Some petechiae (small red spots that do not disappear when the skin is pressed, which are caused by broken capillaries) can appear at this point, as may some mild bleeding from the mucous membranes of the mouth and nose. The fever itself is classically biphasic or saddleback in nature, breaking and then returning for one or two days.
The diagnosis of dengue is typically made clinically, on the basis of reported symptoms and physical examination; this applies especially in endemic areas. However, early disease can be difficult to differentiate from other viral infections. A probable diagnosis is based on the findings of fever plus two of the following: nausea and vomiting, rash, generalized pains, low white blood cell count, positive tourniquet test, or any warning sign (see table) in someone who lives in an endemic area. Warning signs typically occur before the onset of severe dengue. The diagnosis of dengue fever may be confirmed by microbiological laboratory testing. This can be done by virus isolation in cell cultures, nucleic acid detection by PCR, viral antigen detection (such as for NS1) or specific antibodies (serology).Virus isolation and nucleic acid detection are more accurate than antigen detection, but these tests are not widely available due to their greater cost. Detection of NS1 during the febrile phase of a primary infection may be greater than 90% sensitive however is only 60–80% in subsequent infections. All tests may be negative in the early stages of the disease. PCR and viral antigen detection are more accurate in the first seven days. In 2012 a PCR test was introduced that can run on equipment used to diagnose influenza; this is likely to improve access to PCR-based diagnosis.
There are no specific antiviral drugs for dengue; however, maintaining proper fluid balance is important. Treatment depends on the symptoms. Those who are able to drink, are passing urine, have no "warning signs" and are otherwise healthy can be managed at home with daily follow-up and oral rehydration therapy. Those who have other health problems, have "warning signs", or cannot manage regular follow-up should be cared for in hospital. In those with severe dengue care should be provided in an area where there is access to an intensive care unit.
Invasive medical procedures such as nasogastric intubation, intramuscular injections and arterial punctures are avoided, in view of the bleeding risk. Paracetamol (acetaminophen) is used for fever and discomfort while NSAIDs such as ibuprofen and aspirin are avoided as they might aggravate the risk of bleeding. Blood transfusion is initiated early in people presenting with unstable vital signs in the face of a decreasing hematocrit, rather than waiting for the hemoglobin concentration to decrease to some predetermined "transfusion trigger" level. Packed red blood cells or whole blood are recommended, while platelets and fresh frozen plasma are usually not.
Prevention depends on control of and protection from the bites of the mosquito that transmits it. The World Health Organization recommends an Integrated Vector Control program consisting of five elements:
- Advocacy, social mobilization and legislation to ensure that public health bodies and communities are strengthened;
- Collaboration between the health and other sectors (public and private);
- An integrated approach to disease control to maximize use of resources;
- Evidence-based decision making to ensure any interventions are targeted appropriately; and
- Capacity-building to ensure an adequate response to the local situation.
The primary method of controlling A. aegypti is by eliminating its habitats. This is done by getting rid of open sources of water, or if this is not possible, by adding insecticides or biological control agents to these areas. Generalized spraying with organophosphate or pyrethroid insecticides, while sometimes done, is not thought to be effective. Reducing open collections of water through environmental modification is the preferred method of control, given the concerns of negative health effects from insecticides and greater logistical difficulties with control agents. People can prevent mosquito bites by wearing clothing that fully covers the skin, using mosquito netting while resting, and/or the application of insect repellent.
















